This post is part of a series of guest posts on GPS by the graduate students in my Psychopathology course. As part of their work for the course, each student had to demonstrate mastery of the skill of “Educating the Public about Mental Health.” To that end, each student has to prepare two 1,000ish word posts on a particular class of mental disorders.
______________________________________________
Evidence-Based Treatments for Excoriation and Skin-Picking by Blair Penn
I will start with a confession. I pick at my scabs and acne. Mentally, I go through a litany of reasons why I shouldn’t do it… It will only make things worse, it’s going to leave a scar, it’s never going to heal, etc., etc. But alas, I give in to the temptation to pick at it anyway.
I’m sure many of you read my juicy confession and thought to yourself, “Big deal, I do similar things.” And you’re right. My infrequent picking isn’t a big deal as, I assume, neither is yours. Picking at scabs, dry skin, or acne is not an uncommon behavior and I would venture to say that the majority of people do it some. However, this practice, as with nearly everything else, can reach an extreme. When this extreme is reached, and individuals’ quality of life is jeopardized, it is known as excoriation.
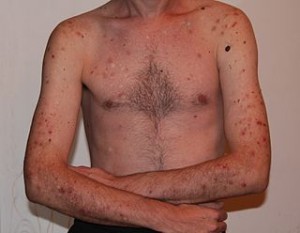 Excoriation, or “skin picking disorder,” is listed in the Obsessive-Compulsive and Related Disorders chapter in the DSM-5. It is also classified as a “body-focused repetitive behavior” (BFRB). Excoriation is the repetitive behavior of picking or scratching at skin resulting in physical or psychological damage. Persons with excoriation often report they are picking at perceived or minor flaws on the skin. The most commonly reported site of picking is the face; however individuals often report having multiple picking sites. It has been estimated that roughly 2% of dermatology patients meet criteria for excoriation.
Excoriation, or “skin picking disorder,” is listed in the Obsessive-Compulsive and Related Disorders chapter in the DSM-5. It is also classified as a “body-focused repetitive behavior” (BFRB). Excoriation is the repetitive behavior of picking or scratching at skin resulting in physical or psychological damage. Persons with excoriation often report they are picking at perceived or minor flaws on the skin. The most commonly reported site of picking is the face; however individuals often report having multiple picking sites. It has been estimated that roughly 2% of dermatology patients meet criteria for excoriation.
What causes someone to develop excoriation? Unfortunately, the general answer is…we don’t really know. There’s a pretty good possibility that genetics are at play somewhere. Several researchers have discovered that persons with excoriation often have a first-degree relative with OCD. Furthermore, excoriation and OCD have a high comorbidity rate. Also, there are animals that have been revealed to pick or chew that their skin, leading researchers to believe that biology is part of the root cause of excoriation. Whatever the cause may be (hopefully soon we will know), it is a distressing mental health issue, and evidence-based treatment is beyond necessary.
Although very few studies have been conducted examining the treatment of excoriation, there are promising options. Pharmacologically, the use of selective serotonin reuptake inhibitors (SSRIs) improved the prevalence of skin picking in case studies, open trials, and double-blind studies, albeit with few participants. Specifically, studies using Fluoxetine, Fluvoxamine, and Naltrexone produced improvements in skin picking. Before excitement settles in for pharmacological treatments and their improvement of the disorder, it is important to take the trade-offs into consideration. Various SSRIs can take anywhere from 4-12 weeks to begin working effectively. For individuals living with such a chronic, debilitating problem one to two months is a lengthy weight for relief. Unfortunately, the side effects of these drugs do not take as long to rear their heads and they do not abate. Side effects of SSRIs include, but are not limited to, nausea, vomiting, diarrhea, and (somehow, considering the previous three) weight gain.
Treating excoriation with medication is certainly a viable option. This treatment, however, is not considered the first-line treatment for excoriation. Rather, therapy is the go-to for many clinicians. Specifically a form cognitive behavioral therapy(CBT) known as habit reversal training (HRT). There are three components to HR, awareness, competing response and social support training. The first session of HRT is dedicated to awareness and is designed like many first-time therapy sessions. It is intended for the clinician to better understand their client. However, unlike talk-therapy, this is done with a very specific goal in mind (not just exploration). Together, the clinician and client work to define skin picking in client specific terms. What triggers my urge to pick? Where do I do it? What is every step involved? Eventually what is known as an operational definition is reached. An operational definition vividly explains the client’s act of skin picking so as to leave no room for question as to what all the act entails. Between the first and second session the client uses this information to self-monitor and keep track of their picking. The competing response training then begins.
Competing response training is much like it sounds. The client is given an act that is completely incompatible with picking. For instance, instead of having your hand available to pick, you are directed to make a tight fist with your hands and hold it for a certain amount of time. Ideally, the competing behavior is performed until the urge to pick subsides and is to be used whenever the urge to pick arises. This process makes the client hyper-aware of their picking as many individuals pick without realizing they are doing so. Social support is pivotal to the success of HR. Thus, individuals intricately involved with the client’s treatment are trained in the HR process. Unlike medication, the effects of HR can be seen near immediately. Thus, it is extremely effective and encouraging for the individual seeking treatment. And, hey, no nasty side effects!
Comprehensive behavioral treatment uses a combination of CBT techniques and HR. Using comprehensive treatment has been shown to be more effective than CBT or HR alone. Using the comprehensive behavioral model (ComB), clinicians can better tailor treatment to their clients’ specific needs. ComB is comprised of four elements: assessment, identify, and evaluation. Assessment in ComB is nearly identical to that of HR; however, the difference in treatments lies in the identification phase. Instead of only being taught an incompatible response to picking, clients are taught to look for sensory substitutes. The clinician and client extensively discuss the sensations that occur during picking and find a substitute that induces such sensations without picking. The clinician and client also work together to alter the environment where picking occurs to make it less conducive to picking. Combining the aforementioned therapies with medication has not been proven to be more effective. Although this article on comprehensive therapy outlines the specifics of treating trichotillomania (hair pulling disorder), the process is the same for excoriation.
While all of us most likely engage in some form of skin picking, there are people who suffer to a damaging degree. While the cause of excoriation is unknown, clinicians and researchers have made huge advances in treating the disorder. Excoriation is not a disease that one must succumb to and it is most assuredly not without treatment options.
